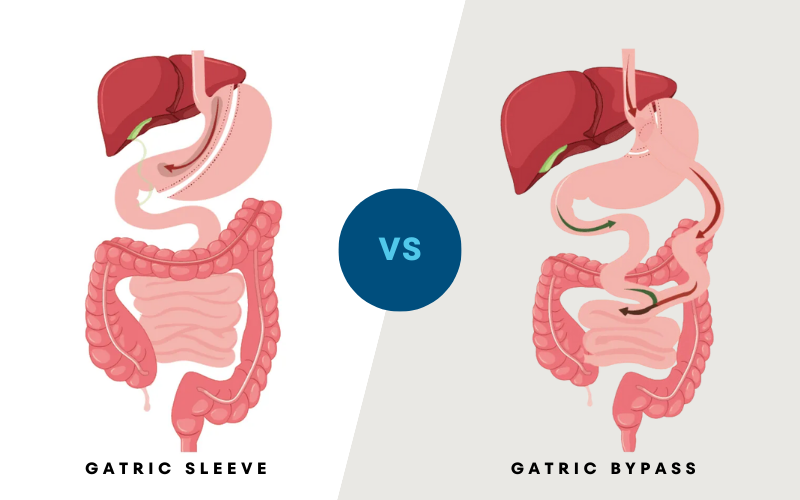
Obesity and Male Reproduction
Reproductive health is an important, but often awkward, topic to discuss.
Sexual dysfunction could be affecting nearly half of male obesity sufferers. Yet due to a lack of clinical awareness and because men might be embarrassed to talk about reproductive health these issues often are ignored and allowed to get worse.
The truth is, male obesity is closely linked to reproductive health; health problems related to obesity like hypogonadism, erectile dysfunction (ED) and infertility can be alleviated by weight loss surgery and positive health behaviours.
In fact hypogonadism (which we’ll discuss below) is shaping up to be a prime target for bariatric surgery on the back of some very positive studies.
Reproductive health risks of male obesity
Male obesity contributes to several serious health problems like type 2 diabetes, low testosterone, depression, and fatigue. These are all related to a condition known as male-obesity secondary hypogonadism (MOSH).
Also called hypogonadism, MOSH is the limited functioning of reproductive organs. Because these organs play an important role in chemical production and regulation, it is vital to address hypogonadism as a symptom of obesity as it is more serious than bedroom performance.
Almost half of all men with moderate to severe obesity are affected by MOSH. In severely obese pre-bariatric surgery patients, that number climbs to 67%.
Signs and symptoms include depression, fatigue, and of course sexual dysfunction although MOSH also impairs fertility, bone mineralisation, cognitive function and fat metabolism.
Put simply, obesity has a significant effect on sex hormone levels.
Enzymes prevalent in the excess tissue of an expanded waistline reduce the amount of testosterone flowing around the body, leading to a slew of related issues.
There is even evidence that testosterone could protect against type 2 diabetes, suggesting a causal link between obesity, MOSH, low testosterone and insulin dependence. Type 2 diabetes in turn affects gonadal testosterone levels and so the vicious cycle continues.
Benefits of bariatric surgery for reproductive health
If you’re uncomfortable talking about sexual dysfunction, you may not get to hear the good news.
Hypogonadism, like several health issues related to male obesity, has been shown to drastically reduce as a direct result of weight loss surgery. Rapid weight loss and the positive lifestyle changes that follow not only increase vitality but also increase testosterone levels and sexual function.
As a result of visceral fat loss sperm count goes up, erectile function is improved in men who were at risk of ED and, with continued physical exercise, testosterone levels steadily increase.
Bariatric surgery might be the most effective way for obese men to tip the scales back in favour of healthy sexual function.
Perth Weight Loss and Surgery help men and women regain their vitality with weight loss solutions including bariatric surgery and tailored after care to stay on track. It is, of course, up to the individual to look after their newfound vitality by sticking to healthier lifestyle habits – but we can help you out.
Contact us online or book a no-obligation consultation to learn more about the weight loss solutions available for you.
It’s time to get serious about how we tackle male obesity and reproductive dysfunction.
Not just for your health, but for a better lifestyle.